Few things make a pet family more anxious than hearing the words “your pet needs surgery.” Whether it is a routine spay or neuter, a dental extraction, or a more complex soft tissue procedure, the thought of your pet going under anesthesia and into an operating room can feel overwhelming. The good news is that veterinary surgery has advanced dramatically, and the tools, monitoring, and protocols available today make procedures safer and recoveries faster than ever before.
At Woodland Springs Veterinary Hospital, we use surgical laser technology for many procedures because it reduces bleeding, swelling, and post-operative pain compared to traditional scalpel surgery. Combined with AAHA-accredited surgical protocols, comprehensive anesthesia monitoring, and individualized pain management, our goal is to give every patient the safest, most comfortable surgical experience possible. If your pet has an upcoming procedure or your veterinarian has recommended surgery, call us at (817) 431-3735 or contact us to discuss what to expect and how we will take care of them every step of the way.
Why Surgical Standards Make a Real Difference
Not all surgical experiences are equal. Anesthesia safety begins with protocols, not just equipment. At Woodland Springs Veterinary Hospital, every surgical patient benefits from a systematic approach that addresses safety at each stage.
Pre-surgical checklist:
- Physical examination to identify any new findings before anesthesia
- Pre-anesthetic bloodwork to assess organ function
- Anesthesia protocol tailored to the individual patient’s age, health status, and procedure type
During surgery:
- Sterile technique maintained from patient preparation through wound closure
- IV catheter placement for fluid support and immediate access to medications throughout the procedure
- Continuous monitoring of anesthesia depth, heart rate, blood pressure, respiration rate, oxygen saturation, body temperature, and end-tidal carbon dioxide
- Immediate response capability for any change in patient status
Post-operatively:
- Recovery monitoring until the patient is fully conscious and stable
- Pain assessment before discharge and at home through the recovery period
- Clear written discharge instructions for every procedure
AAHA accreditation means these standards are evaluated against the most rigorous veterinary practice criteria. Fewer than 15% of veterinary practices in the US and Canada meet AAHA standards. Our surgery services cover a wide range of procedures, including spays and neuters, stenotic nares and elongated soft palate corrections, orthopedic procedures, soft-tissue repairs, growth and mass removals, and gastrointestinal surgeries.
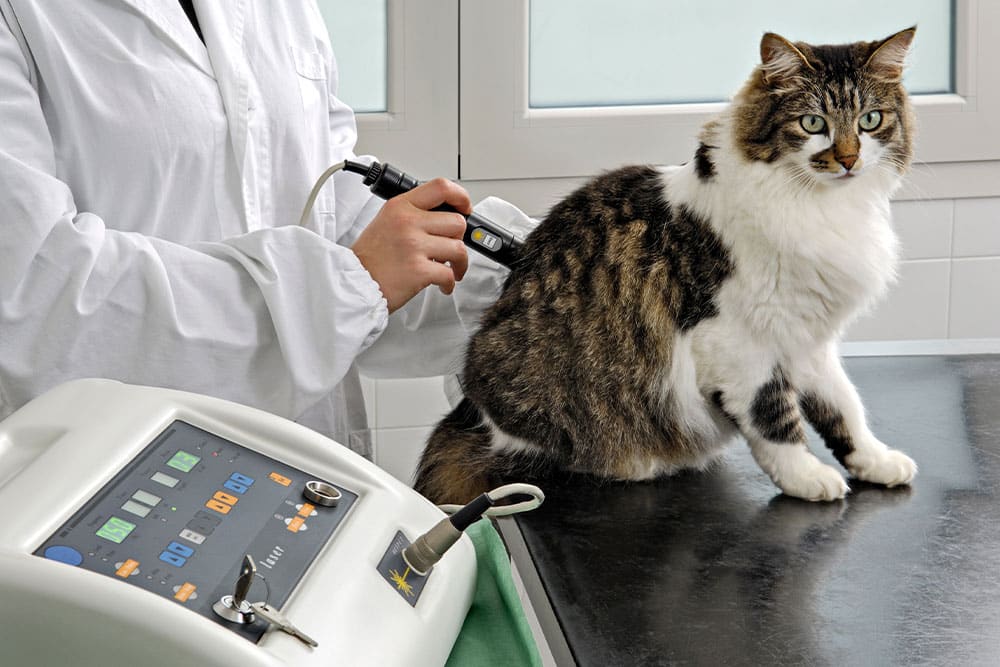
Surgical Laser Technology: Why It Matters for Your Pet
How Laser Surgery Works
Surgical lasers use a concentrated CO2 laser beam to simultaneously cut tissue, seal small blood vessels, and close nerve endings as the incision is made. This simultaneous sealing is what produces the meaningful clinical differences families notice in laser-assisted patients.
Compared to scalpel surgery, laser surgery produces:
- Less bleeding: vessels are sealed as the laser cuts, significantly reducing intraoperative blood loss
- Less swelling: reduced tissue trauma means less inflammatory response in the surrounding area
- Less post-operative pain: sealing nerve endings at the cut reduces immediate pain signals
- Lower infection risk: the laser beam sterilizes the tissue surface as it cuts
- Faster recovery: less trauma and pain typically translates to quicker return to normal activity
We use the laser routinely for soft tissue procedures including spays and neuters, mass and growth removals, oral surgery, and orthopedic procedures. For flat-faced breeds with breathing complications from stenotic nares or elongated soft palates, our brachycephalic laser surgery uses CO2 laser precision to remove tissue from the nostrils and shorten the soft palate with significantly less swelling than conventional surgery would produce, which matters enormously in airways already compromised by anatomy.
Before Surgery: Preparation and Diagnostics
Pre-Anesthetic Bloodwork
The importance of bloodwork before anesthesia cannot be overstated. A young, apparently healthy dog can have underlying kidney, liver, or metabolic abnormalities that would not cause symptoms in daily life but significantly affect how they metabolize anesthesia drugs.
Pre-anesthetic panels assess:
- Kidney and liver function, which govern how anesthesia drugs are processed and eliminated
- Red blood cell count, relevant to oxygen delivery during and after surgery
- Blood glucose and electrolyte balance
- Platelet count and basic clotting parameters
Results guide whether the original anesthesia protocol is appropriate, whether adjustments are needed, or whether the procedure should be rescheduled pending investigation of an unexpected finding. Our in-house diagnostics include same-day bloodwork processing and digital radiography, and three of our doctors have advanced or intermediate ultrasound training when imaging is part of the surgical workup.
What to Expect the Morning of Surgery
We will provide specific pre-surgical instructions for your pet’s procedure. Standard preparation includes withholding food after 10 pm the night before (small amounts of water are typically fine until a few hours before), arriving at the scheduled morning drop-off time, and confirming any medications your pet takes. Our team reviews your pet’s history and bloodwork, confirms the surgical plan, and walks through what the day will look like before pickup later that afternoon.
Pain Management: Before, During, and After
Pain management in pets at Woodland Springs Veterinary Hospital is multimodal, meaning it uses several different methods simultaneously rather than relying on a single drug.
Pre-emptive pain management: medications given before the incision reduce the nervous system’s pain response during and after surgery. Pain signals that are never initiated do not need to be suppressed after the fact.
Intraoperative analgesia: local nerve blocks, NSAID medications, and opioid-based analgesia are used based on the procedure and patient profile.
Post-operative discharge medications: oral pain management continues at home through the critical first days of healing. Clear instructions on dosing schedules and what to expect are provided at discharge.
Laser therapy: reduces inflammation and swelling at the surgical site, decreases pain, and accelerates tissue healing. Multiple sessions in the days following surgery produce measurable improvements in comfort and healing speed, particularly for orthopedic and joint procedures and brachycephalic airway surgery.
Acupuncture: available as a complementary therapy that supports surgical recovery, helps manage chronic pain conditions that may be aggravated by procedures, and provides drug-sparing pain relief for patients who cannot tolerate certain medications well.
Long-term pain support: for patients with concurrent arthritis or chronic pain, monthly Librela injections for dogs and Solensia injections for cats can be incorporated into the broader pain management plan during the recovery period and beyond.

Recovery: Recognizing Problems Early
Red Flags That Warrant a Call
We’ll send you home with detailed instructions and let you know what to expect. If you have any questions, call us. We’re here to help.
Normal in the first 24 to 48 hours:
- Mild lethargy from anesthesia
- Reduced appetite on the first day
- Minor swelling or bruising at the incision site
- Some reluctance to move or change positions
- Fewer bowel movements
Call us or seek emergency care for:
- Excessive swelling, redness, or discharge at the incision site
- Bleeding from the surgical site beyond a very minor amount
- Significant lethargy or inability to rise on the second or third post-operative day
- Fever: feeling hot, shivering, or a rectal temperature above 104°F
- Vomiting or diarrhea that persists beyond the first day
- Difficulty breathing at any point
- Signs of significant pain: vocalizing, guarding the incision, inability to get comfortable
Our emergency care services and team are available for post-surgical questions during business hours.
At-Home Recovery: Setting Your Pet Up for Success
The Physical Environment
Creating the right recovery environment reduces complications and helps your pet heal on schedule.
For dogs: surviving crate rest is genuinely challenging with active dogs, but the crate serves a real purpose. Limiting movement prevents incision stress, jumping accidents, and the overactivity that reopens healing tissue. Keep the crate in a room where household activity continues so your dog does not feel isolated. Food puzzles and chew-appropriate enrichment provide mental engagement without physical exertion.
For cats: post-op care for cats involves creating a quiet, accessible space with litter box at floor level, food and water nearby, and a comfortable resting surface. Cats in pain often seek high spots; removing access to elevated perches during recovery prevents jumping injuries.
The E-Collar Is Not Optional
An e-collar or cone worn consistently is the single most important element of incision care at home. Licking introduces bacteria and frequently tears sutures, converting a healing incision into an infected wound that may require a second procedure to repair. Making the cone more comfortable with padding around the rim and adjusting sleep positions helps with compliance. The collar comes off only for supervised activity.
Daily Incision Checks
Once daily, gently examine the incision in good light. You are looking for: increasing redness beyond the first day, warmth that seems to be intensifying, swelling that is expanding rather than stable, any discharge (small amounts of clear fluid are normal; yellow, green, or significant bloody discharge is not), and whether sutures remain intact.
Discharge instructions will specify whether any cleaning is needed and what products are appropriate. Do not apply any product to the incision without specific guidance.
Frequently Asked Questions
How long will my pet need to be restricted?
Recovery timelines vary by procedure: routine spay or neuter is typically two weeks of activity restriction; more complex soft tissue procedures may require four to six weeks. Your discharge paperwork will include a specific timeline for your pet’s procedure.
When can my pet go back outside?
Leash-only outdoor access for bathroom purposes is standard until sutures are removed. No running, jumping, swimming, or off-leash activity until cleared by our team.
My pet is eating less after surgery. Should I be concerned?
Mild appetite reduction on day one is normal as anesthesia wears off. By day two, most pets return to eating normally. Persistent anorexia beyond 36 to 48 hours warrants a call.
Will my pet need to stay overnight?
Most routine procedures at Woodland Springs Veterinary Hospital are same-day, with morning drop-off and afternoon pickup. More complex surgeries or patients needing extended recovery support may need overnight support, and we will discuss expectations and options with you when scheduling.
Surgery With Care at Every Step
At Woodland Springs Veterinary Hospital, surgery is never routine in the sense of being taken lightly. Every patient receives individualized attention from pre-surgical preparation through recovery, and every family leaves with the information they need to support healing at home.
Contact us at (817) 431-3735 to schedule a surgical consultation or ask questions about an upcoming procedure.





Leave A Comment